Can CT Scans Be Used to Quickly and Accurately Diagnose COVID-19?
Berkeley Lab researchers are working to improve the accuracy of CT scan diagnosis
June 1, 2020
By Linda Vu
Contact: cscomms@lbl.gov
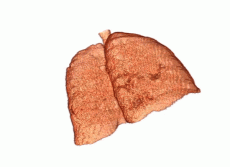
Ushizima and her collaborators are developing a method to narrow the search area on a CT scan or chest X-ray just to the lungs, then detect the lung lesions. (Image courtesy of Daniela Ushizima, Berkeley Lab)
To safely reopen the American economy, most experts agree that we need aggressive diagnostic testing for COVID-19. That way we can isolate known cases, trace their contacts, and quarantine anyone who might be exposed until they clearly show no signs of infection. And when it comes to COVID-19 testing, one big question is whether we should use computed tomography (CT) scans for frontline diagnosis.
At the height of the COVID-19 pandemic in Wuhan, Chinese doctors were using CT scans, which combine a series of X-ray images taken from different angles around the body, to diagnose hundreds of people per day. But the American medical community is so far skeptical. While CT scans do capture abnormalities on the lungs of COVID-19 patients, many other infections look very similar, and doctors worry that this may lead to false-positive and false-negative diagnoses.
This problem inspired Lawrence Berkeley National Laboratory (Berkeley Lab) data scientist Daniela Ushizima to explore whether image recognition algorithms and a data analysis pipeline can help accurately distinguish COVID-19 abnormalities in CT scans and chest X-rays from other overlapping respiratory illnesses, such as influenza, H1N1, other SARS viruses, and MERS.
“Before the pandemic, I was already working with researchers at the University of California, San Francisco, to develop image recognition algorithms for early detection of cancer tumors in the body. We’ve developed algorithms that can search CT scans of different materials. Although the problems aren’t exactly the same, I believe I can leverage these efforts to help classify COVID-19 specific lesions in CT scans and chest X-rays,” said Ushizima.
Studies have shown that CT scans have over 90% success rate at capturing the hazy white spots on the lungs or “ground glass,” a telltale sign of COVID-19, in emergency room patients that have been exhibiting symptoms for two or three days.

Original CT cross-section (left); ground-truth of lesions (middle); automatic algorithm using MSDnet (right) (Image credit: and
Meanwhile, research shows that the widely used reverse transcriptase polymerase chain reaction (RT-PCR) test—a.k.a. the swab test—which detects genetic material specific to the SARS-CoV-2 virus that causes COVID-19, could have a 30% or higher false-negative rate due to human error. To ensure diagnostic accuracy, some countries are supplementing their RT-PCR tests with CT scans.
Ushizima ultimately hopes that her work will produce a method for detecting this “ground glass” in real-time. She’s been working toward this goal with medical researchers at UCSF, San Francisco Veterans Affairs Medical Center, and Thomas Jefferson University since March. And in those two months, they’ve passed some pretty big milestones. Two of their big achievements were developing a method to narrow the search area on a CT scan or chest X-ray just to the lungs, then detect the lung lesions.
“CT scans of the chest actually cover a wide area, creating really big datasets. So to make sure you’re looking at an abnormality on the lung and not the back of the throat, you need to narrow the search area,” said Ushizima. “This reduces the search space early on the analysis process.”
The team is also working to collect and consolidate high-quality, anonymized, and publicly available chest X-ray data into a central database. Relevant databases will eventually be stored at computing facilities that are part of the COVID-19 HPC consortium. Because time is of the essence for increasing diagnostic testing, researchers around the country will be able to access this data through a portal and use it to test their image recognition algorithms.
“In March, when I started working on this, just finding publicly available data for research was a huge challenge. A lot of people were frustrated. But as the pandemic worsened, people became more willing to share data. The problem now is finding high-quality data to teach our machine learning algorithms; there is so much variation in CT scans,” said Ushizima. “Data is where the collaboration with medical schools is so vital; in addition to their medical knowledge, they’ve been a vital resource for helping to guide us toward obtaining IRBs, or International Review Board approvals.”
She adds, “this is science for life. Never has the world been so urgently in need and waiting for more diagnostic testing. We don’t know if our algorithms will be the answer, but we’re working really hard and around the clock to find out.”
This research is supported by Berkeley Lab’s Laboratory Directed Research and Development (LDRD) program. In March, Berkeley Lab mobilized quickly to provide LDRD funding for several research projects to address the COVID-19 pandemic. Other collaborators in this project are Kenny Higa and Robbie Saddre from Berkeley Lab, Duygu Tosun, Jason Crane, and Sharmilla Majumdar from UCSF, medical students Crystal Lee, Jacob Garcia, Spencer Liem and Dr. Baskaran Sundaram from Thomas Jefferson University, and Daniel Pelt from the Centrum Wiskunde & Informatica (CWI), a national research institute for mathematics and computer science in the Netherlands.
About Berkeley Lab
Founded in 1931 on the belief that the biggest scientific challenges are best addressed by teams, Lawrence Berkeley National Laboratory and its scientists have been recognized with 16 Nobel Prizes. Today, Berkeley Lab researchers develop sustainable energy and environmental solutions, create useful new materials, advance the frontiers of computing, and probe the mysteries of life, matter, and the universe. Scientists from around the world rely on the Lab’s facilities for their own discovery science. Berkeley Lab is a multiprogram national laboratory, managed by the University of California for the U.S. Department of Energy’s Office of Science.
DOE’s Office of Science is the single largest supporter of basic research in the physical sciences in the United States, and is working to address some of the most pressing challenges of our time. For more information, please visit energy.gov/science.









